The Key Factors that Cause Psoriasis
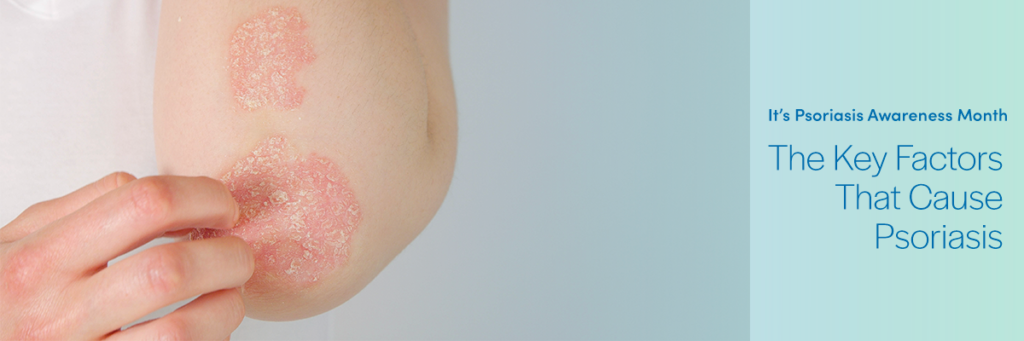
Psoriasis is a multifactorial, auto-immune disease. The exact reasons behind psoriasis are still unclear.
The condition has a strong genetic background. Research suggests that an interaction between genetics and the immune system is one of the primary reasons behind the condition. Some common triggers can worsen the symptoms of psoriasis. The impact of these triggers varies from one person to another.
The Link Between Psoriasis and Genetics
Having a family member with psoriasis enhances your level of risk for the condition. However, people with no family history of psoriasis can still be diagnosed with the disorder. Research conducted on psoriatic skin shows the presence of gene mutations (called alleles).
However, the presence of alleles alone cannot cause a person to develop the condition. Genetic studies have identified 25 gene variants that can increase the risk of psoriasis. The studies indicate a person’s risk level in developing psoriasis.
- If one parent has psoriasis, then there is a 10% chance for the child to have the condition.
- If both parents have psoriasis, the risk is over 50%.
- If you have a relative with psoriasis, then the chances of being diagnosed with the condition are over 30%.
The specific method through which psoriasis passes from the parent to the child is not entirely understood.
The Interplay between Genetics and the Immune System
When the immune system encounters a foreign body such as a virus or bacteria, the T cells respond. The body builds proteins that are involved in the identification of molecules called antigens.
When a person has psoriasis, the gene mutations cause the T cells to identify their skin cells as foreign and attack them incorrectly. The body makes new cells more often than required. The additional skin cells pile up on the surface of the skin and thus cause psoriasis.
Other Contributing Factors of Psoriasis
The National Psoriasis Foundation (NPF) has revealed that at least 10% of people inherit genes that can cause psoriasis. But only 3% of people develop the condition. When external triggers combine with genetics, the chance of developing psoriasis is high. Some of the external factors are,
Stress
The connection between stress and psoriasis is like a loop. Psoriasis causes stress. Stress causes inflammation and increased activation of the immune cells. This results in a psoriasis flare-up.
Skin Injury
Bruises, bumps, and other forms of injuries can irritate your skin and set off the immune system. As a result, the injured portion of the skin becomes the site of a psoriasis flare-up.
Weather
The National Psoriasis Foundation suggests that cold and dry weather can trigger psoriasis. Some studies support the intake of Vitamin D supplements to regulate the immune system during winters.
Drugs
Certain drugs like antimalarials, aspirin, beta-blockers can aggravate psoriasis.
Gut Health
When the bacterial ecosystem in your gut is dysregulated, “leakiness” in the gut can be observed. This triggers inflammation through the entire body and causes the development of psoriasis.
Infections
Infections such as COVID 19 can trigger psoriasis through systemic inflammation. The most common infectious trigger of psoriasis is strep throat.
Lifestyle Habits
Smoking is said to flare up psoriasis by over 60%. The nicotinic receptors in the T cells of the immune system regulate cell activity. The nicotine present in cigarettes can interfere with the functions of the receptors.
Get Help with Treating Psoriasis
Appropriate treatment measures can control the symptoms of psoriasis.
We are profoundly aware of the physical and psychological impact of psoriasis. We offer customized treatment plans to relieve patients from their discomfort and to get clearer skin. Contact us today if you notice any signs of the condition.





